Three early promising Covid-19 innovations that didn’t work.
Clinicians meant well, but research did its thing.

Early in the Covid-19 pandemic, we had nothing more to offer patients than the “usual care.” If patients needed oxygen or intensive care to support them while their bodies fought, we provided that. That’s all we had.
We didn’t know some steroids worked (we now know they help some and hurt others). We didn’t have effective monoclonal antibodies (which basically no longer work on the newer variants). We didn’t have antivirals (some of which work, albeit they’ve mostly been studied in unvaccinated people). We also did not know what didn’t work. Trying some of these ideas was reasonable—if a little quixotic.
At the same time, a handful of non-drug interventions gained rapid popularity among doctors looking to help Covid-19 patients survive. Three ideas in particular seemed promising. We now know that none of them work.
•••
In emergency departments, general hospital floors, and intensive care units, two moves quickly became common. The first was simply placing patients having difficulty breathing on their stomachs facing the floor instead of the usual position of having them rest on their backs facing the ceiling. What parents of infants call “tummy time,” healthcare workers call the “prone position.”
Proning, it was thought, would help oxygen reach parts of the lungs where the then-novel coronavirus was taking up shop. It was believed that proning patients would decrease the likelihood they would end up in comas on mechanical ventilators. Now, two years later, research in JAMA Internal Medicine suggests proning doesn’t work—and maybe even causes harm. After reading the paper, I’m not convinced proning causes harm, though. (The way the study was designed makes that inference a little murky.) And yet, there are reasons the hint of harm seen in some patients may be real (as opposed to a reflection of other factors that were baked into the study). One particularly scary proposal advanced by the study’s authors is that while proning did improve oxygenation to at-risk areas of the lung, doing so actually prevented or slowed the natural course of the disease. That temporary increase in oxygen levels may have actually made a patient’s clinical deterioration harder to detect, delaying a much-needed escalation of critical care. If true, clinicians essentially tried to game immunology and lost.

The prone position was hoped to increase air movement to the back of the lungs. It may have. But it didn't help Covid-19 patients, as hoped. (Image source: Wikipedia)
The second idea floated early in the pandemic involved constructing a guard thought to keep medical teams safe while placing patients on breathing machines (mechanical ventilators). That procedure, called intubation, is “aerosolizing,” meaning it causes the patient to exude a lot of air—and with it, a lot of virus. Doctors theorized that enclosing the head of the patient in a Plexiglass cube to contain the air around the patient might protect everyone else in the room from that air. The idea caught on.
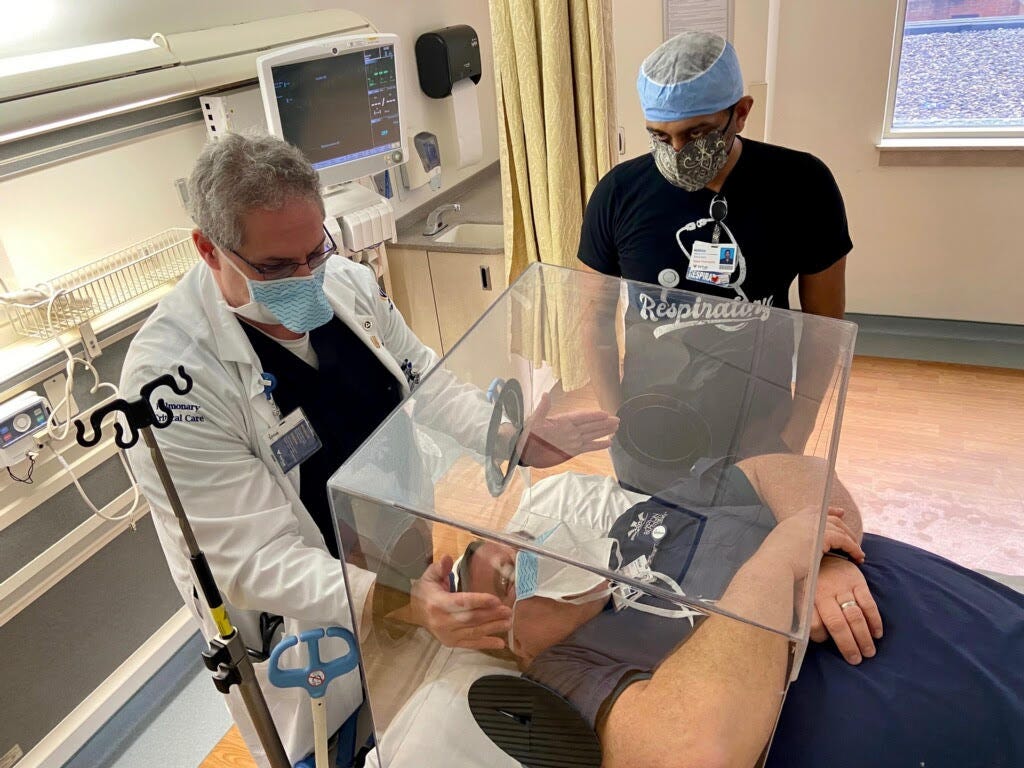
Innovations like this "intubation safety box" did not keep medical providers safer, and may have backfired. (Image source: Wikipedia).
Soon, emergency departments and ICUs everywhere were using these boxes routinely. But the boxes didn’t help. Research subsequently showed the boxes slowed down the procedure, which can worsen outcomes. Worse, apparently, the air in the boxes billowed out of the sides, likely exposing medical teams to more of the virus than if the air just rose directly to the ceiling vents. Before long, we had shelved those boxes.

A portable device that measures oxygen levels. Seems like a great idea. But did it help anyone with Covid-19? Research suggests that the answer might be no. (Getty Images).
Another idea that gained popularity early in the pandemic: Asking Covid-19 patients well enough not to need hospitalization to use portable oxygen monitors. A remarkable feature of Covid-19 is that many patients develop very low oxygen levels, called hypoxia, well before they appear to be in any medical distress. This is known as silent hypoxia, or even “happy hypoxia.” Enter wireless portable pulse oximeters. These “oximeters” are worn on a finger and they measure the real-time oxygen level of the patient. The idea was that if patients wore these at home and knew when their oxygen levels were dropping, they’d know to go back to the hospital for care before things got much worse. It seemed like a great idea. But, yet again, subsequent research published in the New England Journal of Medicine failed to show that it helped. Patients given oximeters didn’t have different rates of hospitalization compared to the control group. Also telling, the number of days in the hospital was not different, meaning that earlier detection of dropping oxygen levels did not stave off complications that prolonged the illnesses. Not only that, the oximeters didn’t even change anxiety levels. The hope had been that since most patients improve, seeing a steady oxygen level might be reassuring.
But it was a wash. While yet another disappointment for a non-pharmaceutical innovation that was hoped to help patients, there’s one caveat here that may mean that these devices may yet have some role to play. The control group didn’t have oximeters, but did have access to video telehealth. That means that trained clinicians had the chance to evaluate the control group patients, at least remotely, before they decided whether to go to the hospital. So really, this study compared oximeters to clinician judgment via telehealth and found no difference. What we don’t know is whether oximeters are actually better than nothing. For this reason, I might still advise Covid-19 patients who have access to these devices to use them, acknowledging their limitations.
•••
Each of these “innovations” suggested early in the Covid-19 pandemic were reasonable, plausible, and even clever. But frankly, that’s not enough. Real-life data can be humbling. That’s why when someone floats a new idea—be it for Covid-19 or anything else—I am always a little skeptical, even if the idea has great intellectual appeal. People come up with lots of great ideas—in theory. The reality is that very few of these turn out to work in practice. It’s worth sorting out which ideas work and which ones don’t. That’s exactly how progress is made. But in my work—and I suspect it is true in many professional fields—I’ve learned that thinking something will work, does not mean it does.
•••
❓💡🗣️ What are your questions? Comments? Join the conversation below!
Follow me on Twitter, Instagram, and on Facebook and help me share accurate frontline medical information!
📬 Subscribe to Inside Medicine here and get updates from the frontline at least twice per week.



