More emergency patients leaving before treatment than ever.
Average time per ER visit has also increased since 2020.
One of the strangest things about the early months of the Covid-19 pandemic was that demand for emergency care decreased, although the severity of illness per patient increased. For weeks and months, gone were our usual “sorta-sick” patients, like those with migraines who badly needed treatment, and a host of other conditions that generally benefit from emergency (if not life-saving) care. For example, with elective procedures canceled, we stopped seeing the usual number of patients with complications. (While complications that send these patients to the ER for evaluation might occur in a small percent of cases, those add up quickly, especially since we see patients who feel unwell after care from every other specialty.)
New data shows how the ERs have changed
There are a number of data benchmarks that reflect the state of affairs in ERs and hospitals in general. Recently, Inside Medicine data guru Benjy Renton showed me some data that tell interesting stories about demand for emergency and hospital-level care before, during, and after the worst of the pandemic. Let’s take a look at two metrics.

Metric #1. ER patients leaving before being fully evaluated.
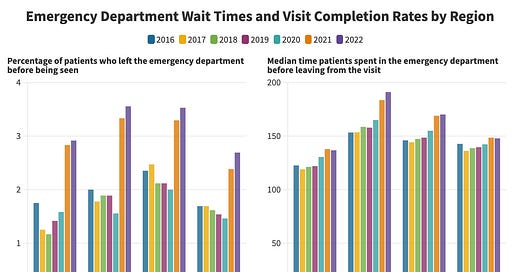
The first (left panel) is the percentage of patients who left ERs before being seen by a clinicians (other than an initial triage assessment) by year from 2016 through 2022. Patients tend to leave ERs before being seen when wait times are excessively long. As you can see (teal bars), 2020 was not a bad year. In fact, the region with the largest decrease in patients leaving before being seen was the Northeast. That makes sense because Covid-19 affected life (and care) in the Northeast a few months sooner than most other places in the US. But then in 2021 and 2022, these rates jumped way up.
It’s not hard to hypothesize the reason for this. Starting in 2021, we had to deal with Covid and everything else. That included a backlog of elective care (including required but technically delayable care that was put off early in the pandemic). Also, in 2022, we saw the return of seasonal viruses like flu and RSV, which came back at higher than usual levels, likely due to a catch-up phenomenon (that is, less herd immunity due to suppressing those pathogens out due to Covid mitigation measures). So, our hospitals were full. When that happens, ERs get backed up too. And, when ERs are full, waiting times go up. When waiting times go up, patients leave. Now you get it!
(And thanks if you already have!)
Metric #2. ER visits are lasting longer.
The other benchmark (right panel) we want to show you is the average amount of time patients spent in the ER per visit by year. This metric reflects three things in particular. First, the stuff we just discussed. More demand means things take longer. The second is acuity of illness. As the graph shows, in 2020 (again, the teal bars), the amount of time patients spent in the ER increased everywhere. When patients are sicker, we need to stabilize them or do more tests to figure out what is wrong with them before moving them out of the ER, either to other parts of the hospital, transferring them to another facility, or sending them home, as appropriate. This tracks with what I remember of that time. Covid patients were not quick and easy cases. (The donning and doffing of PPE in the pre-vaccine era was a whole production, and that was just one of many small ways that added up to things taking longer than usual.) Third, getting certain patients out of the ER in 2020—those with psychiatric emergencies, for example—often meant sending them to a place that was equipped to accept them. Some would take Covid patients but had limited space. Delays. Others would only take Covid-free patients, but we had to prove that with negative tests, tests that sometimes took hours or longer to get results on. Delays. So, even though overall patient volumes were lower in 2020, things took longer that year.
Then, in 2021 and 2022, average time spent in the ER jumped up (in most places), due to a combination of everything we’ve discussed. Another influencing factor here could be staffing changes. Some places downsized their clinical staff after 2020-2021, and others have had turnover, meaning some providers know their internal systems less well.
(Learning something? Please share Inside Medicine!)
Still safe, if slower.
I don’t want you to worry that ERs can’t provide timely life-saving care. In fact, I think what’s happening is that because we focus on the sickest patients first—of whom there are somewhat more than in the past, owing to these issues and the aging population generally—it’s the somewhat less acutely ill patients who are affected by longer waits and visits.
When patients complain to me about how long things are taking, I always apologize for that and remind them that safety comes first, speed second. People understand that, but they don’t love it. Trust me, we’re on the same page!
Have you noticed changes like the ones described here? Please contribute your experiences in the Comment Section!
Thanks to Benjy Renton for curating this Data Snapshot!



This is probably the dumbest question ever - but what will it take for hospital administration to hire more people to care for the growing needs that you list in the article? Maybe you should interview them on one of your podcasts - if they would agree to be interviewed.
Tangential to Seneca Plutarchus (and to your post): Shortly pre-pandemic, my wife fell on the ice and broke her wrist. After almost three hours in the ER waiting room, with a friend advocating for her (I was out of town) but still not having been either seen or even interviewed, she thought to call her primary practice for advice. They had no facilities to treat her, but told her that the hospital in whose ER she was waiting also has a walk-in clinic at their orthopedic facility a couple of miles away. Her friend immediately drove her there (so she became a "left before treatment" statistic), where she was seen within minutes and treated quickly. The break was set by the (50-something) PA who is in charge of the clinic, but with the supervision and approval of the orthopedic surgeon (30-something), who said the PA had done hundreds of them (20 years as an army medic), many more than she had. The bones were so well set that in the end no surgery was required. - But the point is that the ER could not even inform my wife of the existence of an alternative. Several physicians have since told us that an ER cannot do anything that might seem to be sending a patient to a facility with a lower level of care - even if that facility is part of the same hospital. (At the time the hospital was affiliated with MGB; it's now a fully integrated part of the MGB system, with the old hospital name replaced by MGB signs everywhere.) - This is clearly a fairly uncommon scenario, but it highlights some limitations of the system. Thanks for your thoughts.