Inside Medicine: Five on Friday (March 22, 2024).
This week in medicine, what I'm thinking about, etc. You know, an actual newsletter.
We are back with “Five on Friday", the feature where Inside Medicine behaves like an actual medical/health/science newsletter. Below are top-of-mind things that I’m thinking about right now. And please vote in the poll at the end!
If you value this feature—and Inside Medicine in general…
Here we go…
Item 1. Havana Syndrome studies come up mostly empty.
Two large studies in the Journal of the American Medical Association came up empty in a search for any objective evidence that the so-called “Havana Syndrome" is an organic illness, as opposed to a psychiatric one. No unusual biomarkers or brain findings were seen above and beyond those found in non-affected controls. These appear to be the best data we have on this saga to date. I’ll write more about this one this weekend, as the intersection between medicine and politics could someday have incredibly important implications.
Item 2. Intermittent fasting data breaks the internet.
A research poster presented at a cardiology conference suggests that intermittent fasting may be associated with increased mortality. This splashy finding received a lot of media attention—unusual, because the findings are not peer reviewed and the data are pretty limited.
I read the poster. It’s extremely limited. I truly have no idea why responsible science media outlets are running with this one. The discussion of the findings in some New York Times coverage highlighted some of the limitations of the dataset, but missed others that are important. Props, though, to Matthew Herper for covering it well in STAT News. As Herper highlighted, the study design does not allow for causation to be established.
But I have other major questions. I’m trying to get more information because, based on my read, the findings could literally be meaningless. It all boils down to how the study was done, and the poster lacks key details I need. From what I can see, though, it looks like this study may just indirectly show that people with advanced cancer die more than others. That is, people with advanced cancer are able to adhere to an intermittent fasting-like diet. So the fact that cancer patients who were not eating much were found to be dying at higher rates does not impress me as evidence about intermittent fasting. My early suspicion is that these data are meaningless (especially since changes in all-cause mortality were not detected in this study).
In general, when we can’t tell whether a study even has a chance to be meaningful, journalists probably shouldn’t be uncritically putting the findings into headlines of major media outlets. (Again, Herper and team wrote a nice headline that did include the words “Oh, come on.” Niiice.)
That said, I’m unsure the data in favor of intermittent fasting are all that great either. It seems like a strategy (possibly an effective one) to reduce energy intake—which is ultimately the cornerstone of most successful diets.
Item 3: Q&A with Dr. Paul Offit.
Long before Covid appeared, Dr. Paul Offit was a pediatrician and scientist who co-invented the rotavirus vaccine. His service on the FDA’s Vaccine and Related Biological Products Advisory Committee during the pandemic put him in the spotlight, in part because, at times, his rigorous reads on the emerging literature led him to cautious (and I believe correct) stances that were not always the knee-jerk yes, yes, yes. In my view, his careful interpretations made him among the most pro-vaccine voices not afraid to go against the grain.
His new book Tell Me When It's Over: An Insider's Guide to Deciphering COVID Myths and Navigating Our Post Pandemic World covers a lot of ground, especially about misinformation. In prepping for our Q&A, I read the book and found it insightful (and only a few areas where I found myself disagreeing).
Here’s the Q&A we did over on MedPage Today. Topics covered include:
Why some vaccines cause “sterilizing immunity” but not others.
The politics (and non-politics) of vaccine hesitancy.
Some wins related to vaccine uptake during the pandemic.
I really enjoyed speaking with Paul, and I think you’ll find it interesting. Here’s that link.
Item 4: The Affordable Care Act turns 14.
Tomorrow marks the 14th anniversary of the Affordable Care Act. The law has made a real difference. Remember, before the ACA was passed, insurance companies could deny coverage to people with pre-existing conditions. Sounds crazy now, but it’s true. And, according to the Biden Administration, up to 100 million people could be denied coverage if the ACA were to be repealed. I’m old enough to remember John McCain standing in the way of a Trump Administration-driven attempt to repeal the ACA. So, at stake in the 2024 election is the fate of this very law.
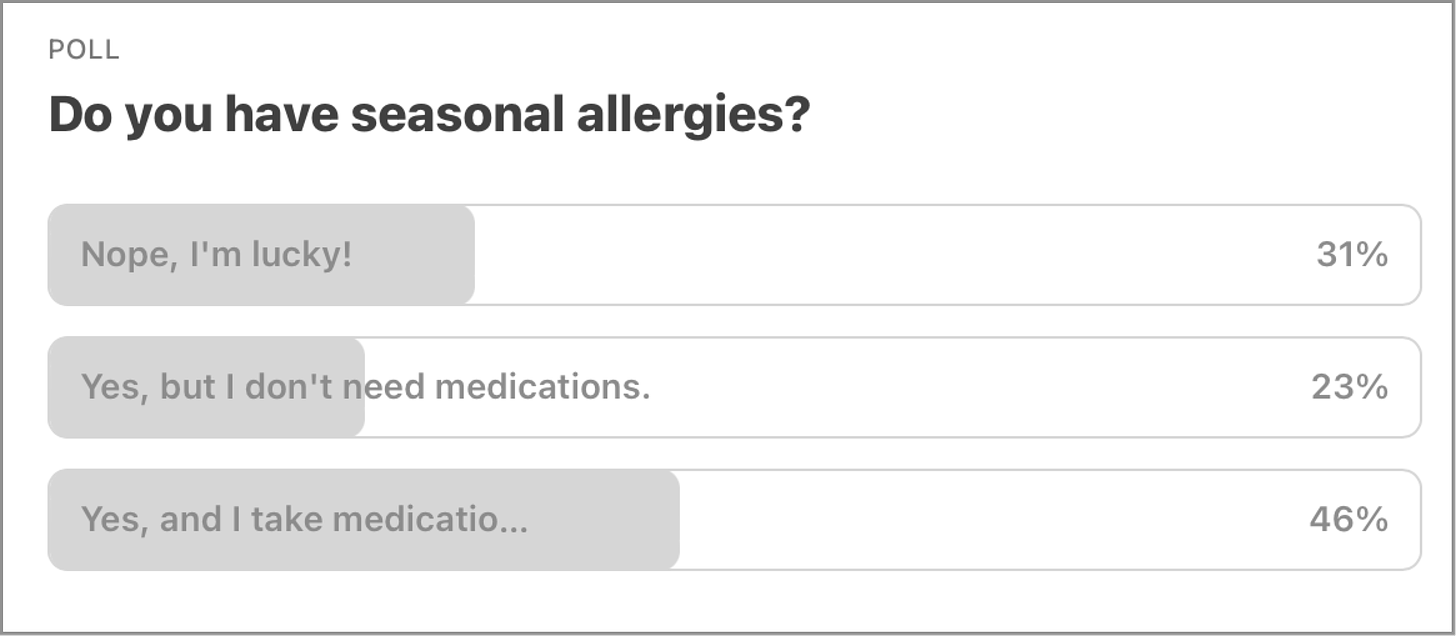
Item 5. Poll of the Week results.
Here are the results of last week’s Inside Medicine poll. That’s a lot of allergy sufferers amongst you! (I’m one of them.) Maybe we’ll do another Q&A with an allergist soon!
Item 5a. Poll of the Week for this week!
And here is this week’s poll. March is Colon Cancer Awareness Month. So…
That’s it. Your “Friday Five!”
Feedback! Do you like the “Five on Friday” format? Have any ideas for next week’s Poll of the Week? Any great articles you read elsewhere that you want to share with the Inside Medicine community? Other musings or thoughts?
Please contribute to the Comments!





Thanks again for your insatiable desire to learn and share. On the anniversary of the Affordable Care Act, I'm good-naturedly laughing at the writing of anything that happened so recently with "I'm old enough to remember...", but it's never a waste of time to remind all that the coming Presidential election outcome could threaten that much needed program. That's not politics, that's an ethical issue. For me it's I remember when there was no managed healthcare, doctors could afford private practices, and then HMO's started, and that led to mismanaged healthcare. My Dad was a CEO in the med insurance biz in the late 1970's in Baltimore, and quit his upper level job because he was being asked to do unethical things. In 1985 I was diagnosed with Progressive MS at 27 and then RA a year later. At that age we barely had time to make ends meet with both working, a 3 year-old child who was very asthmatic and got pneumonia every winter, let alone accrue savings. My husband needed to switch jobs to advance and move into a job closer to his true profession. We were scared to death the new job would find out about his very sick wife. Our HMO did not let us go to a good specialist and we had to go to Johns Hopkins out of pocket for my first visit to the neuro that diagnosed the MS. Fortunately, my personnel director was able to switch us to a better plan (for more $$) instead of having to wait for a formal enrollment period. Not likely to happen today. All my life we had to be careful to hide my disability from my husband's co-workers and bosses for fear he would lose his job or be bypassed for promotions. I got sicker and lost my ability to work a full time job income, while getting assaulted by massive healthcare costs even while paying insurance premiums. Thank god for Obamacare addressing pre-existing conditions for women (unlike me) who are sick or have sick children and are abused by their husbands who carry their health insurance so they stay in that abusive relationship. And the ACA made sure more people are insured. For those of us who had older children at the time who were still dependents finishing undergraduate work full time, they could still be covered by their parents' plan till age 25 thanks to ACA. Things have become much worse for medical staff and even worse for their patients as we move to private equity firms and CEO's running our healthcare, but am so grateful for the ACA. (And I'll be lighting a birthday candle for the ACA). But we've still got a long way to go.
I very much liked 5 on Fridays!