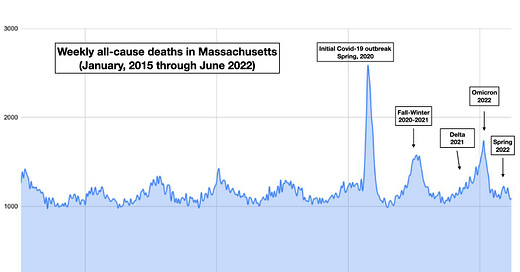
Good news on excess mortality in Massachusetts.
Despite a Covid wave, from a mortality standpoint, things looked normal this past spring.

Today, my colleagues and I published a new paper in the medical journal Lancet Infectious Diseases—and it actually contains some good news. From the end of February of this year through the end of June, there were no more deaths from all causes than usual in Massachusetts, despite over 226,000 new Covid-19 cases. During previous waves, from the initial cataclysmic outbreak in 2020, to Delta, to the early Omicron wave, whenever cases would rise, increases in all-cause mortality quickly followed.
That didn’t happen this spring, in Massachusetts at least.
This uncoupling of “excess mortality” from Covid-19 case counts is remarkable and unusual. It implies that, at least temporarily, those at the highest risk of dying due to Covid had high levels of protection from fatal outcomes. While all-cause mortality is not the only metric we need to watch, it’s an extremely valuable one for measuring where we are in the pandemic.
Consider the major Covid-19 waves up until now:
During the initial spring wave in 2020, around 14,600 deaths would have been expected during the same 13-week stretch in a normal year. Over 22,600 occurred, a 54% increase. During the worst three weeks, rates were more than double that.
During the worst of the Fall, 2020-Winter 2021 wave, around 24,000 deaths would have been expected during the same 20-week stretch in a normal year. Over 27,400 occurred, a 14% increase.
During the Delta wave, around 22,100 deaths would have been expected during the same 20-week stretch in a normal year. Over 24,000 occurred, a 9% increase.
During the initial 8 weeks of the Omicron wave, nearly 10,000 deaths would have been expected during the same stretch in a normal year. Over 12,200 occurred, a 22% increase.
During the 18 weeks of the spring 2022 wave, 20,500 deaths would have been expected during the same stretch in a normal year. Just over 20,600 occurred. Even if that change were statistically significant (which it wasn’t) it would be a 0.7% increase. That’s an improvement.
Now, in May and June excess mortality crept up. But even then, the increase (around 5%) wasn’t statistically significant. That said, I suspect that may reflect the limitations of our model because the numerical rise in excess mortality followed the largest rise in cases we recorded all spring. Still, a 5% increase in all-cause mortality pales in comparison to prior waves.
Why did this happen? There are many possibilities. First, Massachusetts is a state with high vaccination rates. But that can’t be the whole story because we had excess mortality during Delta and Omicron, and vaccination and booster rates didn’t suddenly go up this spring. (Fourth doses were not common enough to explain our findings, it seems). Next, during the initial Omicron wave, the virus tore through the state (like everywhere), infecting droves. While the disease caused great harm, we expect that those who recovered do have something to show for it: short-term protection against infection (weeks to a few months, perhaps) and longer-lasting protection against severe disease from a future infection. That means the odds of fatal outcomes in high-risk demographics may have improved for a time; for example, a high-risk person who got Covid in January who had a 4% chance of dying at that time might have had less than a 1% of dying during a spring re-infection as a result of their earlier infection (and perhaps a 4th dose). How long that protection lasts we don’t know. Another explanation—a sickening one—is that the population that survived into spring was simply harder to kill than the one that entered the winter wave. Experts call this a “healthy survivor effect.” Many who died during the Delta and early Omicron waves had pre-existing conditions and were at high risk of dying from Covid if they caught it. Sadly, many of those individuals are gone now. However, over time, the surviving population will again become more vulnerable, as always. For example, Covid has worse effects in people with cancer or organ transplant recipients. Every day, more people enter those risk pools. Covid awaits them. During the spring, there were temporarily fewer vulnerable targets for Covid to kill, resulting from the winter tsunami.
That said, there were still over 9,400 hospitalizations of patients with Covid-19 in Massachusetts during the spring and over 1,100 deaths chalked up to Covid. Does this contradict our lack of excess mortality finding? Not really. Some people will claim that the 9,400 hospitalizations were “incidental.” While the ratio of people hospitalized “for” Covid-19 to “with” Covid-19 has increased over time, many misunderstand what that means. Most so-called incidental Covid-19 hospitalizations are not patients with broken bones that happen to have Covid. Rather, most Covid-related hospitalizations reflect dangerous non-Covid emergencies which Covid likely either directly caused, or else was a simultaneous “2nd hit” that the patient couldn’t absorb. I’ve been calling this the “Covid tipover” since last year. So, the lack of excess mortality in the spring here mean that infections were significant enough to tip the scales to requiring hospital-level care, but not dire enough to be lethal.
And what about those 1,100 Covid-19 deaths? Does the lack of excess mortality during the spring mean those were not really caused by Covid-19? It’s impossible to say. Sure, it could be some degree of “deckchair rearrangement.” Determining the underlying cause of a death, especially in medically complex people, is actually pretty subjective. (That’s why excess mortality is a less biased pandemic metric). Absent the pandemic, a similar number of people would have died this spring from other causes, and chalked up to cancer or heart disease, say. Through that lens, the fact that 1,100 people died with Covid could be seen as incidental (i.e., unrelated). I suspect that’s part of the story. But also, our model probably underestimates excess mortality due to that healthy survivor effect I mentioned. It’s not just that there are fewer old people around (we do correct for that). It’s that the pandemic has killed more 75-year-olds who had 0-5 years of life remaining, than those with 6-10 or more. We just don’t know who’s who, nor the ratio. So, it could be that there really was more death than there “should have been” this spring—albeit still far less than prior waves. Indeed, that we saw a lot of “Covid tipover” during both Delta and early Omicron and excess mortality tells me that what changed this spring was that the surviving population was healthier and carried far more Covid immunity.
Does this mean the pandemic is over? No. First, the effect looks temporary. It does appear that excess mortality again occurred in Massachusetts in July and August—albeit at lower levels compared to prior waves. That means high-risk people in particular will likely benefit from fall boosters. Second, interpreting the presence of excess mortality is asymmetric. Whenever there is excess mortality, there’s no discussion to be had. Things are bad whenever there’s all-cause excess mortality. But when there isn’t excess mortality, there could still be signs that Covid remains a threat, and that the pandemic cannot be shrugged off. That’s why following hospitalizations and Long Covid (although that’s harder to track) continues to matter.
Did you like this? Share it! Better yet, upgrade to Premium and get exclusive articles, audio versions of articles, interviews with big names in medicine and health, and access to the Inside Inside Medicine community on Facebook, where I answer questions and more.
❓💡🗣️ What are your questions? Comments? Join the conversation below.
Follow me on Twitter, Instagram, and on Facebook and help me share accurate frontline medical information!
📬 Subscribe to Inside Medicine here and get updates from the frontline at least twice per week.
Acknowledgements: I wish to thank my co-authors on the Lancet Infectious Diseases paper: Benjy Renton, Alexander Chen, Chengan Du, Chenxue Liang, Shu-Xia Li, Zhenqiu Lin, and Harlan Krumholz, as well as the Registry of Vital Records and Statistics, Office of Population Health, Massachusetts Department of Public Health.