Field Notes: Ruling out a broken bone without x-rays.
I'm an ER doctor miles away from an ER. Can I still practice medicine?
Greetings from the west coast of Mexico. As I wrote the other day, we have a medical kit here with provisions that can handle a number of situations that might come up.
A couple days ago, my skills were put to the test. Thankfully, it was nothing life-threatening—just a kid with a twisted ankle. But the child was in a lot of pain. Naturally, I took a look and wanted to be helpful, if I could be.
Evaluating ankle trauma is pretty straightforward, even in austere settings. What everyone else wants to know is whether there’s a broken bone. While that’s on my mind, it’s not remotely my first concern.
The first thing I want to know is whether there are signs of an injury compromising the blood flow or causing damage to any nerves in the region. If so, that usually means there’s a very badly dislocated bone (which may or may not be broken). Regardless of anything else, I want to find my way around that joint and that bone, and put things back into place (setting the bone) as quickly as possible. How to do this depends on the bone, the joint, and the injury pattern. “Reducing” a dislocated bone can be simple or not.
The next thing I want to know is whether anything else is going on (other than the obvious injury). If there’s ankle pain, I’ll leave the ankle for last; that way, we won’t forget anything. I ask questions about the rest of the leg. Is there pain in the shin? Knee pain? Thigh or hip pain? Back pain?
I also make sure I understand why the injury happened. When a kid falls playing sports, there’s not much more to glean. But when an older person falls while walking, I want to know whether something else caused the fall. Did they feel dizzy or light-headed prior to the fall? Was there chest pain? In other words, is something medical going on in addition to the orthopedic injury? If so, we’d address those issues too. Depending on the person, or the setting, there are umpteen other considerations.
In this case, there were no signs of a serious vascular or nerve injury, and the fact pattern of the twisted ankle was typical (i.e., a kid being a kid). I was looking at isolated, mild ankle trauma. Now, my task was to determine whether this child needed to go to an ER or clinic for x-rays, either to diagnose a broken bone or to rule that out.
I applied a simple “decision tool” called the “Ottawa Ankle” criteria. Based on what I found, I was confident that there was not a broken bone (note: broken bones and fractures are interchangeable terms). That meant no need for an x-ray and no long trip to an ER. This was a sprained ankle, and not a particularly bad one. Whew!
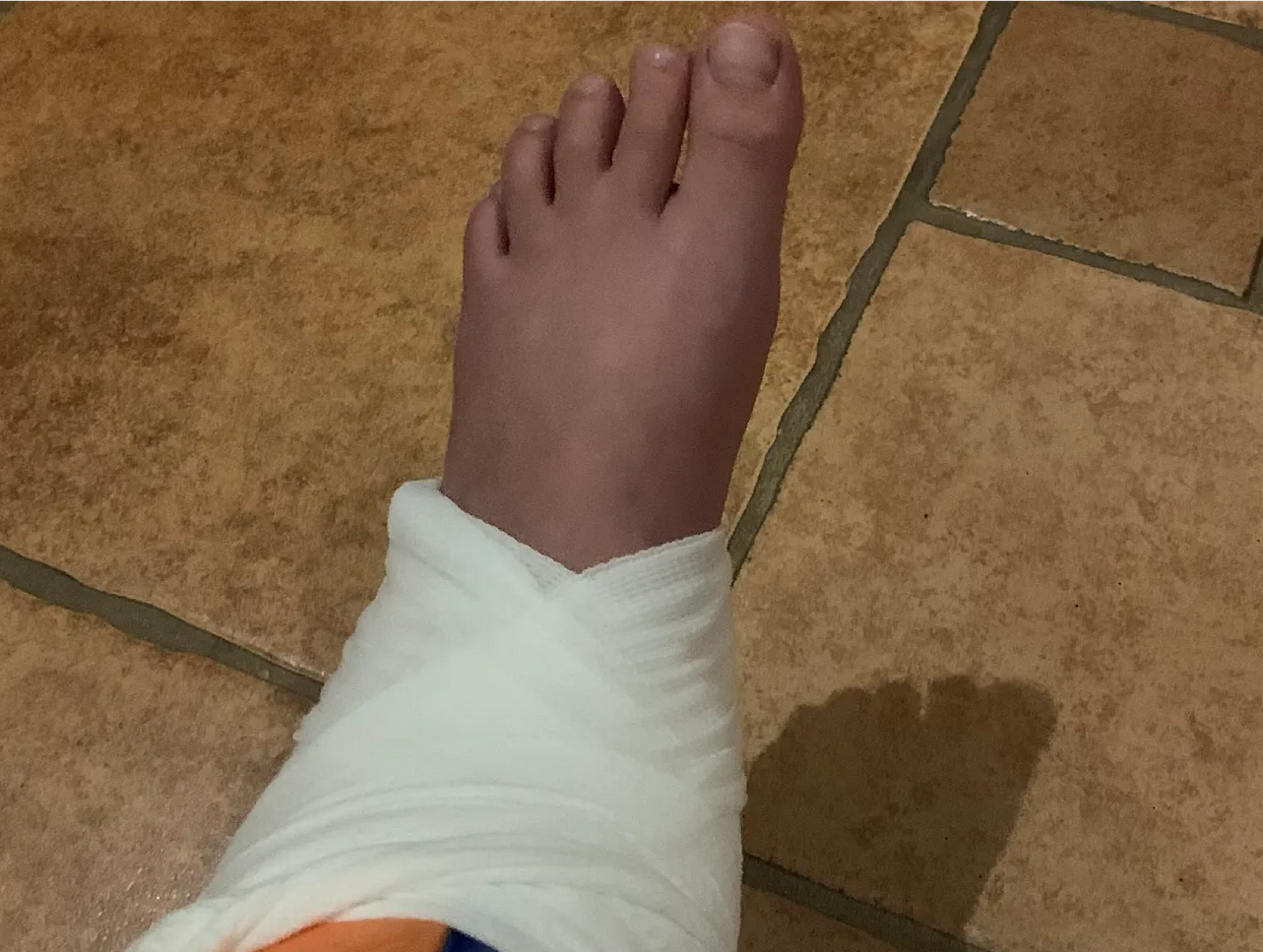
The treatment plan was simple. Ibuprofen, ice and heat (whichever felt better), elevation, compression (an ace wrap would have been fine; we had something a little more advanced), and “taking it easy” (which meant that the kid could put weight on the ankle and walk, as tolerated).
But—just for a second—I had a moment of self-doubt. After all, the Ottawa Ankle criteria (which I have applied hundreds of times, probably) was tested and validated in emergency department patients, not random kids out in the middle of nowhere. Could I really apply the same rules to a patient who was in a vastly different setting from the one where the protocol was derived and proven?
Yes, I decided, I could. After all, we apply the Ottawa Ankle criteria in children whose ankles are messed up enough to warrant trips to the ER. That means the population we routinely us the criteria on is comprised of patients who are far more likely to have broken bones than one who, say, happened to twist an ankle within a few hundred feet of a friendly, traveling ER doctor. I was on solid ground. Over the next day or so, I watched as things improved, which was great to see.
I often wonder how useful I really am, outside of ERs, where I have tools and teams to work with. So, it was nice to be able to be useful out here.


Educating the public by demystifying science and medical doctoring likely comes at a cost.
I really enjoyed reading this.
Thank you
I was in Mexico 50 years ago on an extended camper van vacation. Far from any medical facility, I got stung by a sting ray on the fat part of my palm. Fat is leaking from the wound and my arm is swelling to my elbow. They brought me to “the guy who treats these things”.
Garlic. Yep. He had me eat it, and he wiped it all over my wound.
Obviously it worked. Wink wink, because I’m here today to tell my tale.