Field Notes: How a young person's "unnecessary" ER visit may have saved a life during the holidays.
Run-of-the-mill cases can have second order effects.
Inside Medicine is a daily newsletter where I bring you to the frontline of medicine and public health. Sometimes, my clinical experiences teach me in unexpected ways, making me a better doctor. Today’s essay is a follow up to an earlier popular post, but with far more specifics. I hope you find it educational, and even inspiring.
(Note: details have been changed to anonymize the patient).
Thanks for reading and supporting Inside Medicine!
My patient was a 20 year-old woman with no important medical problems. She had symptoms of an upper respiratory infection that seemed pretty mild overall. She had been seen in an urgent care clinic a couple days prior, tested for influenza, Covid-19, and RSV (all negative) and sent home with some decongestants.
But she wasn’t feeling better. She’d had a fever on and off for 4 days, which was longer than usual when she gets seasonal viruses, she noted.
On physical examination, her vital signs were normal—no fever, even (she’d taken some Tylenol before coming in). Her breathing was fine.
Still, I ordered a chest x-ray. Why did I do this? Why did the results potentially save a life—albeit not hers?!
Why did I order the chest x-ray? I ordered the chest x-ray based on a principle, one that is not necessarily taught in medical school or residency—although I am sure I picked this up from a mentor during my residency training.
The basic premise is that if a patient has already sought out care and been treated in some manner, and they are now seeking care again, the patient has fallen out of the “normal way of things.” By that, I mean that patients—especially young and healthy ones—usually get better regardless of whether we prescribe anything, be it simple or fancy. For the most part, patients are rational people. They don't come to the ER for funsies, nor the subpar turkey sandwiches. So, when a patient decides to seek another opinion a few days after an initial one, my general rule is to “do something more” than the last care providers did. This is not to say that the first clinicians were wrong or incompetent. But with the benefit of more time and more information—including the very fact that the patient is seeking out further care, which only occurs in a small minority of cases—I may be able to solve a small medical mystery that had been murkier just a couple of days earlier.
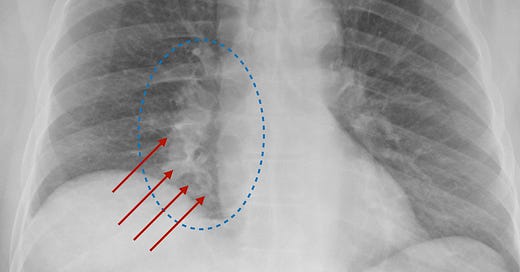
What were my patient’s results? My patient’s chest x-ray showed what looked to be a fairly straightforward case of bacterial pneumonia in the right lung. That meant that antibiotics were indicated.

Now, I am not so arrogant to think that I saved this patient’s life. While pneumonia can indeed be deadly, the truth is that most of the time, healthy people who get bacterial pneumonia probably clear the infections spontaneously, and without the aid of antibiotics. But even among the young, occasionally, a few cases get worse, and can even become life threatening.
Do I think I saved this patient’s life by catching her brewing bacterial pneumonia? Not really. But the next thing that happened may have saved a life.
“Are you going home for the holidays? Will you be around anyone who is medically vulnerable?” I asked her. She would be, she said. She would be seeing her grandmother, who had some medical problems.
The hairs on my arms went up. Diagnosing this pneumonia might not have saved the life of the patient in front of me. But it very well may have saved her grandmother.
It was an important reminder for me, as a physician. Run-of-the-mill cases can have second order effects.
So, in addition to prescribing antibiotics (which would make her less contagious within a day or two), I advised her to wear a mask when she was anywhere near her grandmother, and maybe keep the windows open (or open them occasionally) to promote air exchange—which we know decreases the spread of many contagious pathogens.
A confession. I used to (metaphorically) roll my eyes about patients going to ERs who did not have anything close to a true medical emergency. Over time, I’ve come to realize that in almost all cases, there’s a legitimate reason that these “low acuity” patients come to ERs.
Sometimes it is a matter of access—we are there 24/7/365, and see all-comers regardless of their ability to pay or anything else. Sometimes it is a matter of fear—someone they know had similar symptoms that were signs of a serious problem. Sometimes it is a matter of feeling that something just is not right. This is not to say that every patient is correct in their assessment of what is going on. But it is to say that they bear being heard very clearly and thought about. The case above adds one more reason that I honestly had not thought of before: to get a timely diagnosis and treatments (and take further action) that might protect others.
So, please remember! Your own health is not always the only consideration when you get sick. If you’re traveling for the holidays this weekend and do not feel well, dropping by an urgent care clinic to get tested for Covid, RSV, and flu (or other viruses they check for) might lead to a diagnosis and treatment that will make you feel better sooner. But perhaps more importantly, you have the opportunity to protect the lives of the people you’re visiting. Wear a mask if you might be sick and isolate, especially early in your illness.
Spread love, not pathogens!



When you talk about “access,” I think you’ve diplomatically sidestepped the issue of the quality of care being provided at the typical urgent care clinic, which in my family’s and friends’ experience is often poor. You brought a level of experience and training to the situation that is far beyond that of the “provider” seen at most urgent care clinics.
I am an exception, but that is because my private internist is part of my local quartenary level medical center’s system, and their express care clinic (same day appointments 7 days a week) is staffed by full-time faculty physicians (sometimes full profs) from one of the academic primary care departments. Fantastic doctors.
A couple of times recently, I had a situation where a trip to the ED would have been reasonable, in fact, in both cases, they debated whether to send me to their ED down the street for specialist care. But they were able to do a quick phone consult with the specialist on call, develop a plan and get me into their specialist’s clinic for follow-up 48 hours later (which would normally take months as a new patient). They had access to all of my charts, as did my internist at my physical 2 months later to be able to check on the status of the problem. Completely seamless care of literally the highest quality level medical care available on the planet (paid for by my insurance). I suspect your system has a very similar setup.
But that’s incredibly far from the reality for most people, who see a random provider at an urgent care factory with no follow-up, paid for by cash.
I think there might be an interesting study to be done to somehow look at what happens at ED visits following outside medical care by either the patient’s regular physician or urgent care. E.g., evaluate admissions for pneumonia between the two groups. Perhaps politically unpopular, though.