Breaking: Flu hospitalized more than Covid at apparent peak of 2023-2024 season.
Plus, more US residents are up-to-date on their flu shots compared to Covid.
We are back with a Data Snapshot and some (we think?) Breaking News.
A quick reminder that we’re on the PBS/NPR model here. Maintaining the Inside Medicine Covid, flu, and RSV dashboard is not free, but it is valued by so many of you. If you’ve already upgraded, thanks! For everyone else, I hope you consider joining the them.
Above all, thank you so much just for being here and have a safe week! —Jeremy
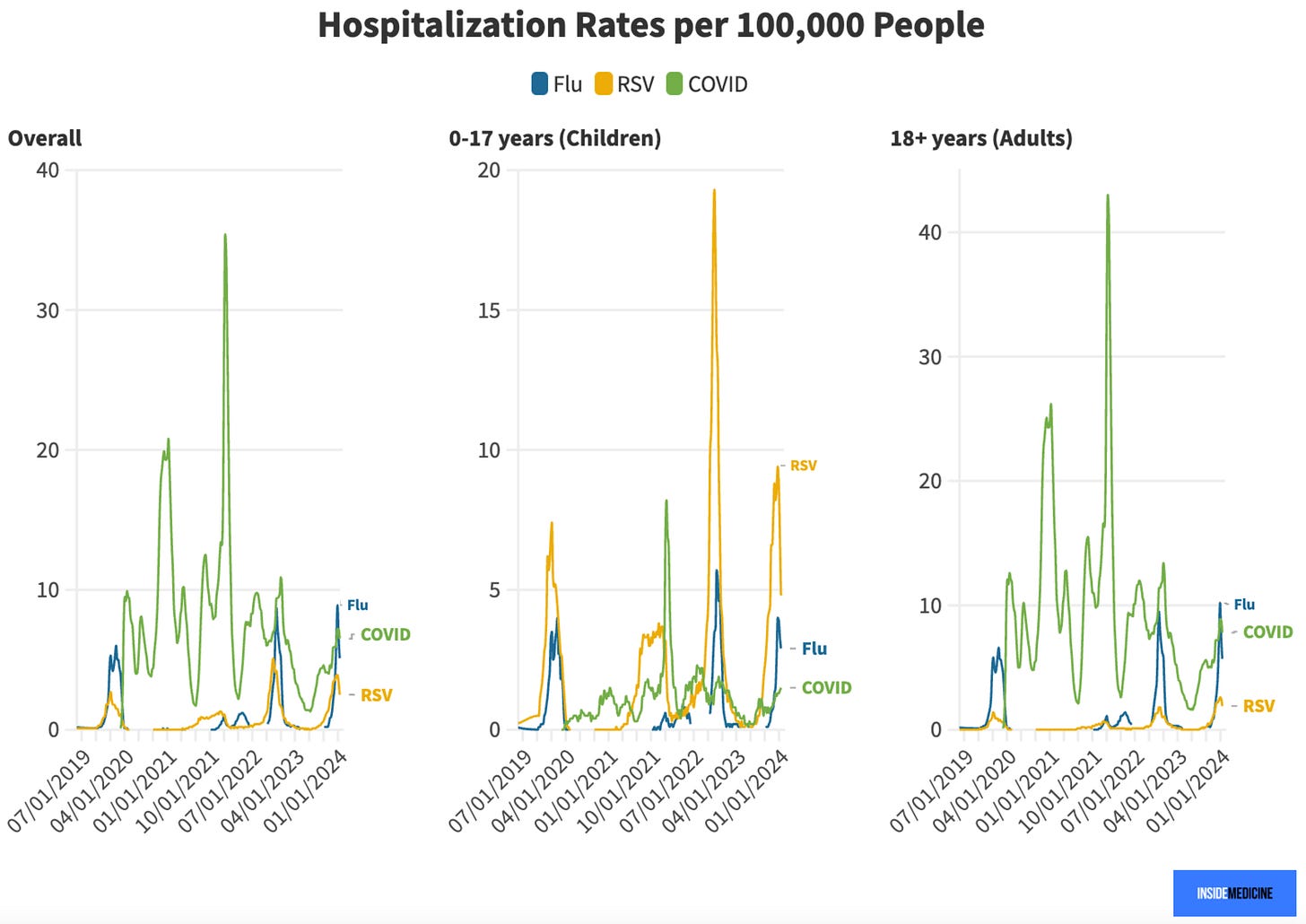
For the first time since the Covid-19 pandemic began, influenza hospitalized more US residents than Covid-19 during the apparent peak of the year’s respiratory illness season. The zenith of cold and flu season looks to have occurred the week ending December 30th. If these data hold up, flu edged out Covid out overall, including among both children and adults. (That said, among children, RSV outpaced both flu and Covid, as it did last year). Here are hospitalization rates per 100,000 people in the United States (i.e., not per infection).
Mortality may turn out to be a different story. For example, many infants and young children are hospitalized with RSV, but only briefly for “airway monitoring.” Very few become gravely ill. And we don’t know enough to make a head-to-head flu/Covid comparison among older adults regarding severity. It’s tempting to infer that Covid-19 remains the deadlier native virus because of how many deaths it still causes or contributes to, but some of what we are seeing may be due to differences in immunity in the older population. The older population has seen flu for over and over for decades. Covid is only in its fifth year. So, I’m not surprised that Covid remains the leader in hospitalizations among people ages 65 and up, and the gap larger among those ages 75+ and 85+ (those data are not shown here, but you can explore everything on the Inside Medicine Covid-19 Metrics Dashboard by clicking here).
Here are weekly hospitalizations from 2019 until now by age groups:
As you may have noticed, RSV hospitalizations dominate over Covid and influenza in young children. In adolescents, flu took over last year as the leading cause of hospitalization among the “big three” viruses, and remains in the lead this year.
But adults is where the really interesting story looks to be unfolding. During the late December peak, flu hospitalized more people than Covid among the 5-17, 18-49, and 50-64 age groups. Meanwhile, Covid hospitalizations are now far lower than analogous points in prior seasons. So it’s not that we are having a particularly bad flu season. Rather, Covid is now hospitalizing fewer people than before. Yes, some of the decrease in Covid hospitalizations may reflect the lack of universal testing, which was far more common a year ago. But I doubt that can explain most of the decrease from last and prior seasons. It’s mostly our immunity (and maybe variant differences, to some extent).
Are vaccination rates playing a role?
Survey data suggest that Covid-19 vaccine rates are quite a bit lower than influenza vaccine rates this season. In every age group, more people have received a flu shot than a Covid-19 shot. Check it out:
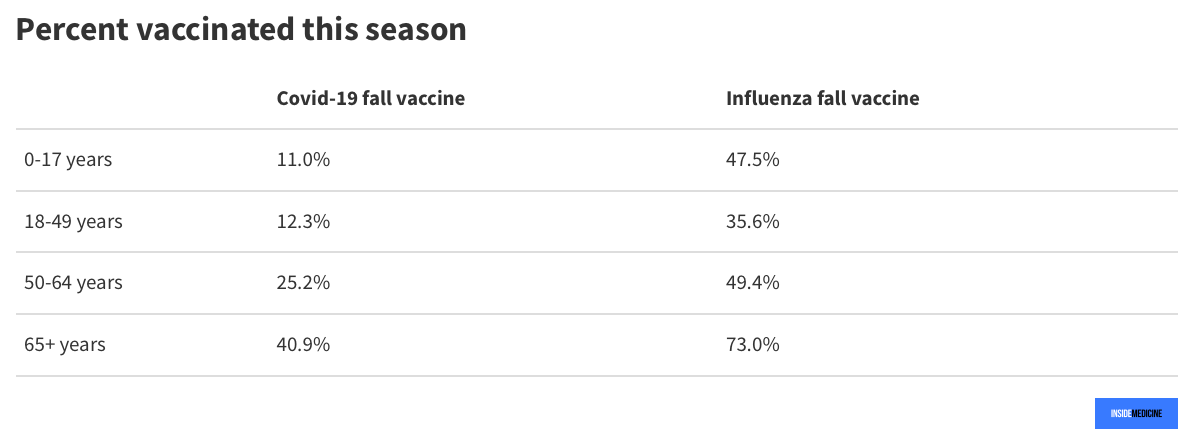
The analysis on this cuts in both directions. In adults ages 18-64, the “native” rate of flu hospitalization would be even higher in comparison to Covid-19, were it not for the higher vaccine rates compared to Covid. Meanwhile, for people ages 65 and up, only 41% have received a Covid shot this season compared to 73% who received flu shots. But keep in mind that many people ages 65 and up have received 6 or 7 doses of Covid vaccines over the last few years. So, again, cumulative immunity may be playing some role here.
A word of caution on inferring severity differences…
I want to emphasize that we can’t be certain when making comparisons between these pathogens based on these numbers alone. It’s possible, for example, that very high-risk subgroups have different vaccination behaviors. For example, it might be that the most vulnerable 10% of the population (who could represent 80% of hospitalizations) are much more likely to be up-to-date on their Covid shots than their flu shots. If that were the case, the rates we are seeing in the graphs could be hiding the fact that Covid remains the more dangerous pathogen. Controlled studies in which patients of similar profiles were carefully matched and compared would more reliably reveal whether flu has truly overtaken Covid as the more dangerous virus out there.
In addition, while Covid continues to show a clear seasonal pattern (worse in winter), it has yet to vanish in the spring and summer, as RSV and flu usually do. So, while flu hospitalizations outpaced Covid at the apparent peak of this respiratory virus season, Covid’s higher “sea level” during the off-season may more than make up for it.
We’ll see.
Nevertheless, the script has flipped compared to prior winters. Early in the Covid-19 pandemic, it was patently obvious that Covid was a much more dangerous disease than flu, both because of its contagiousness and on a per-case basis. The severity gap has closed over time, but even last year during the 2022-2023 season, Covid appeared to retain its claim as the more dangerous pathogen.
I’m not sure that remains the case in 2024. The data we’ve been looking at hint at a reversal—but this is nowhere near definitive. The real answers likely vary by person, based on age, medical risk factors, and individual immune histories.
But there’s this, at least: When comparing Covid and flu, it used to not be complicated. Covid was worse, by far. Now these analyses are requiring much more nuance and subtlety.
Is that something like progress?
Here’s our metrics dashboard link again.
Thanks to Benjy Renton for curating and maintaining the Inside Medicine dashboard.





I would have never thought that the flu would surpass covid19 hospitalizations. Yet here we are. Even with more vaccinated with the flu vaccine than the covid19 vaccine. I know we just started 2024. It will be interesting to see how the percentages change by the end of the year.
I think this is a very important post and I'm surprised there are so few comments: it does feel like progress to me. That said, sometimes I think the hospitals are almost willfully blind: we sent over a covid + patient with lab abnormalities, and the ED just didn't acknowledge the Covid diagnosis. I still consider Covid a more lethal virus than flu--and the weekly deaths don't compare, right?