New study poised to make emergency intubations--a difficult but lifesaving procedure--safer.
Your "Five on Friday" lead story for June 21, 2024...
We are back with “Five on Friday", the feature where Inside Medicine behaves like an actual medical/health/science newsletter. Also, please vote in the poll at the end!
If you value this feature—and Inside Medicine in general…
Here we go…
Item 1: Making emergency intubation safer.
One of the most common lifesaving procedures emergency physicians perform is placing patients on mechanical ventilators. We do this by sedating and temporarily paralyzing patients so that we can put a breathing tube into their windpipe. This is called intubation.
I pride myself on being both one of the better and least prolific intubators among my emergency medicine colleagues. Why do I think I am any good? Because I always have the sense that there’s a bit more time than it may seem. So, I use that time to “optimize.” That is, I do things that improve a patient’s ability to get oxygen while getting prepared for intubation. One thing I like to do if there’s time is to use “non-invasive” ventilation to actively push more oxygen into a patient who is in respiratory distress than a standard oxygen mask can supply. I’ve been doing this my entire career (whenever possible), based on teachings from master clinicians I was lucky enough to train with. (Oh, and the reason I am among the least prolific intubators is that by the time I have optimized the conditions for the procedure, it sometimes turns out that the patient no longer needs to be placed on the ventilator; And for those who still need it, they have the best conditions possible.)
Now there is finally high-quality data to support my practice. A new large clinical trial published in the New England Journal of Medicine found that patients who were randomized to receive non-invasive ventilation instead of a standard oxygen mask had a lower incidence of dangerously low oxygen. I’m hoping that this study will render non-invasive ventilation before intubation as the new standard approach, rather than something that only some of us try to do when possible. It might even stave off a few intubations altogether.
Item 2: Dr. Fauci speaks out on his own terms.
Recently, we’ve seen Dr. Anthony Fauci hauled out before Congress and generally maligned for being imperfect during the pandemic. While indeed nobody is perfect (and there have been places where I think he either got something wrong or could’ve been right sooner), my impression of him is that he’s a highly intelligent person who served the public with enormous distinction during his career.
That’s why it’s nice to hear him speak out on his own terms. An excerpt from his new book (which I have just started to read) entitled “On Call: A Doctor’s Journey in Public Service,” appeared in The Atlantic this week. In it, Dr. Fauci described his attempt to remain helpful during the early Covid-19 response, in the face of President Trump’s obvious misunderstanding about what was going on and what to do about it. I’ll be reading this book in the coming weeks. (If you are considering doing the same, please vote in the weekly poll below!)
Item 3: Residency interviews by Zoom? It’s permanent.
With the Covid-19 pandemic raging in the fall and winter of 2020-2021, US residency programs (the hospital-based training programs that take newly minted physicians and train them for their chosen specialty) turned to virtual interviews for the first time. What many assumed would be a one-off for just that year has now become the permanent standard in many places. Turns out that job interviews on Zoom (or similar platforms) are just as useful for both applicants and program directors for getting the information needed to make important decisions—and a lot less expensive. My own program does virtual interviews only now. Some places have returned to in-person interviews.
In my role as editor for the Annals of Emergency Medicine’s News and Perspective section, I recently commissioned an article about how virtual interviews are going these days. Now that we’re a few years into this era, are residents who matched into programs they only ever saw via Zoom happy? Are the program directors who recruited these candidates equally satisfied? For the most part, the answers are yes and yes.
And the carbon footprint difference is not trivial either. Research shows that a typical medical student who has to fly around the country for multiple residency interviews can easily add over 30% of their annual CO2 emissions (and maybe higher, depending on where they live and other factors) from these trips alone. There are also equity issues and other considerations. I found this all pretty interesting (says the editor). If you’d like to hear more about this from both the perspective of newly minted doctors and the educators who recruited them into their hospitals for training, check it out!
Item 4: June is National Gun Violence Awareness Month.
In the US, firearms are the leading cause of pediatric mortality. Around 10% of all firearm-related fatalities in the US occur among those ages 19 years and younger. This scourge affects far too many children, but Black children are four times more likely to be killed by firearms than White children. We can do so much better. Here is the link to these and other important facts, from Sandy Hook Promise—an organization that hopefully should not have to exist forever, but clearly is very much needed now.
Item 5: Poll of the Week.
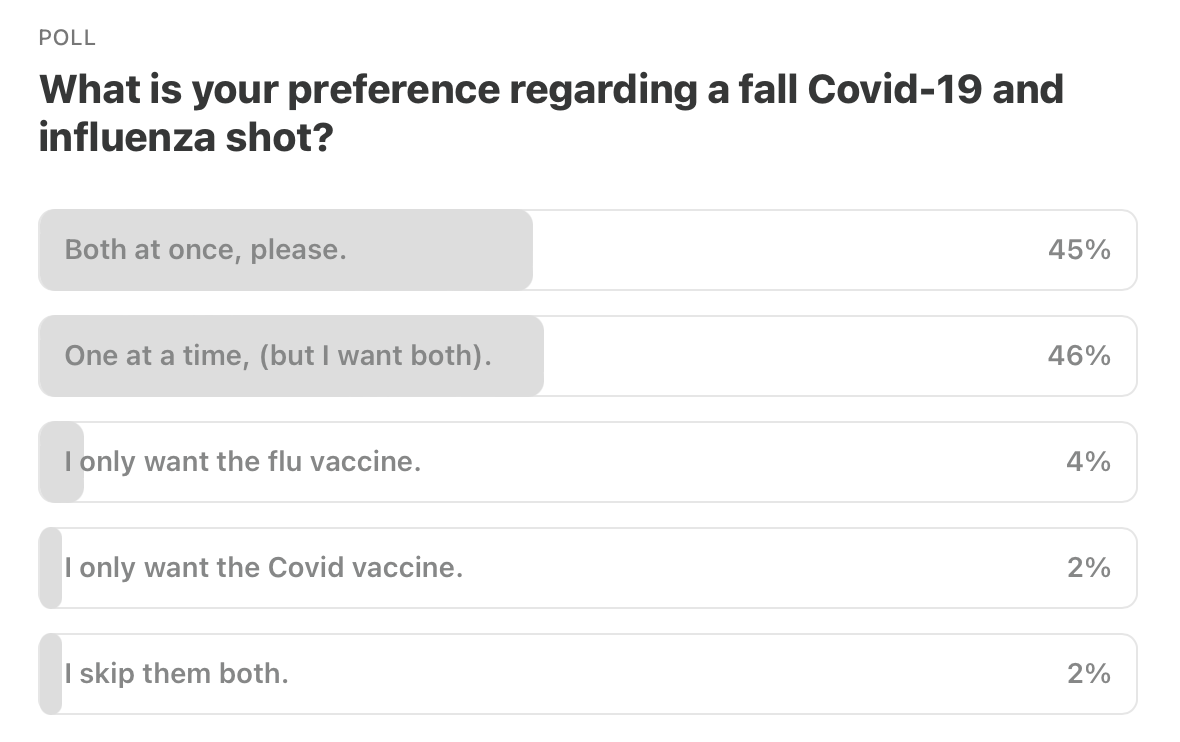
Here are the results from last week’s poll. Thanks for your votes!
Item 5a: Poll of the Week for this week!
I’m looking for more ways to engage you, the amazing Inside Medicine community. Would an occasional “Book Club” be of interest? I would choose an appropriate book about medicine/health/science (generally from one of the Big Five publishers) and we’d read it over a few weeks. We’d then meet via a Zoom webinar to discuss the book—perhaps with the author present, if we’re lucky—and take your questions and feedback. If there’s interest, I’m thinking that Dr. Fauci’s book could be the first choice. Please vote and add your comments/ideas about how this might work best for you.
That’s it. Your “Friday Five!”
Feedback! Do you like the “Five on Friday” format? Have any ideas for next week’s Poll of the Week? Any great articles you read elsewhere that you want to share with the Inside Medicine community? Other musings or thoughts?
Please contribute to the Comments!





The impacts of climate change on mental health - what to know and what to take into consideration when making health decisions: https://www.prevention.com/health/a60986884/climate-change-causes-brain-changes/
Love the book club idea. I am asking you (selfishly) to write about nurses and their paths in our current environment as our daughter is in a four year nursing program. We are flying blind as parents as we want her to hopefully get offered a job where she will be well trained, mentored at a responsible hospital.